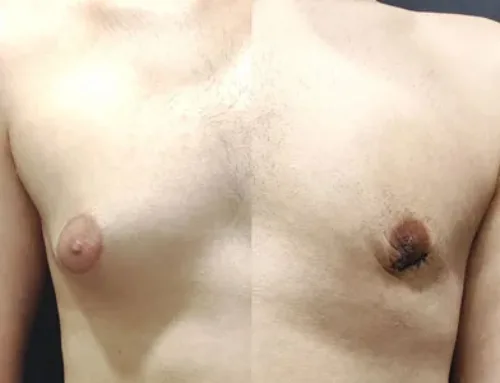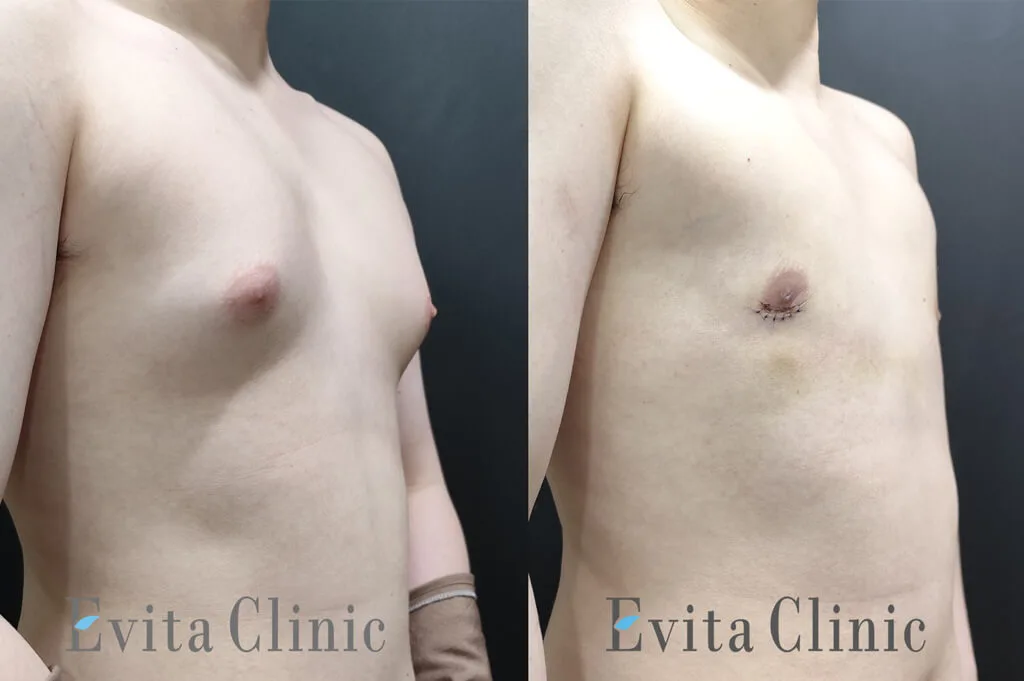
Adolescent Gynecomastia Surgery (Age 16) – Grade II Gynecomastia
After 2 weeks
This case involves a 16-year-old adolescent patient with persistent gynecomastia that first developed around the age of 14.
During puberty, temporary breast enlargement in males is relatively common due to hormonal fluctuations. In many cases, the glandular tissue decreases naturally within 1–2 years. However, in this patient’s case, the glandular tissue remained unchanged even after more than two years of observation, indicating persistent gynecomastia.
Because the condition did not improve and continued to cause significant psychological discomfort, the patient and his guardian decided to proceed with surgical treatment.
Preoperative Condition
The patient was diagnosed with Grade II gynecomastia, characterized by:
- Moderate enlargement of the male breast
- Firm glandular tissue beneath the nipple
- Visible projection of the nipple-areolar complex
- Mild chest contour imbalance
Although the patient had a relatively slender body frame, the glandular breast tissue created a noticeable feminine chest contour, making the condition more apparent.
More importantly, the patient experienced psychological and social distress due to the condition. He reported feeling uncomfortable in situations such as:
- Participating in sports activities
- Changing clothes in locker rooms
- Wearing light clothing or tight shirts
Over time, he developed a habit of hunching his shoulders and chest forward in an attempt to hide the chest contour.
Surgical Procedure
The surgery was performed under IV sedation (sleep sedation) and took approximately 2 hours.
Procedure details:
- Small peri-areolar incision
- Liposuction chest
- Direct excision of glandular breast tissue
- Careful contouring of the chest
Excised glandular tissue:
- Right side: 42.4 g
- Left side: 40.4 g
The removed tissue consisted of dense glandular breast tissue, which explains why the enlargement did not regress naturally over time.
Postoperative Photos
The postoperative photographs shown above were taken during the patient’s second postoperative visit, before suture removal.
At this early stage of recovery:
- Mild swelling and bruising may still be present
- The incision sutures are still visible
- The final chest contour will continue to improve as healing progresses
Even at this early stage, the chest contour has already become noticeably flatter and more masculine compared to the preoperative appearance.
Posture After Surgery
In the postoperative photos, the patient still appears to slightly hunch his chest forward. This is a common habit developed by many gynecomastia patients who have spent years trying to conceal their chest.
This posture often improves gradually as patients regain confidence after surgery. With time, and especially through regular exercise such as chest muscle strengthening, the patient is expected to develop a more natural and confident posture.
Insurance Coverage in Korea
In Korea, persistent gynecomastia with confirmed glandular tissue may be covered by the National Health Insurance system, particularly when the condition persists after puberty and causes functional or psychological distress.
In this case, the surgery was performed with guardian consent, which is required for surgical treatment in minors.