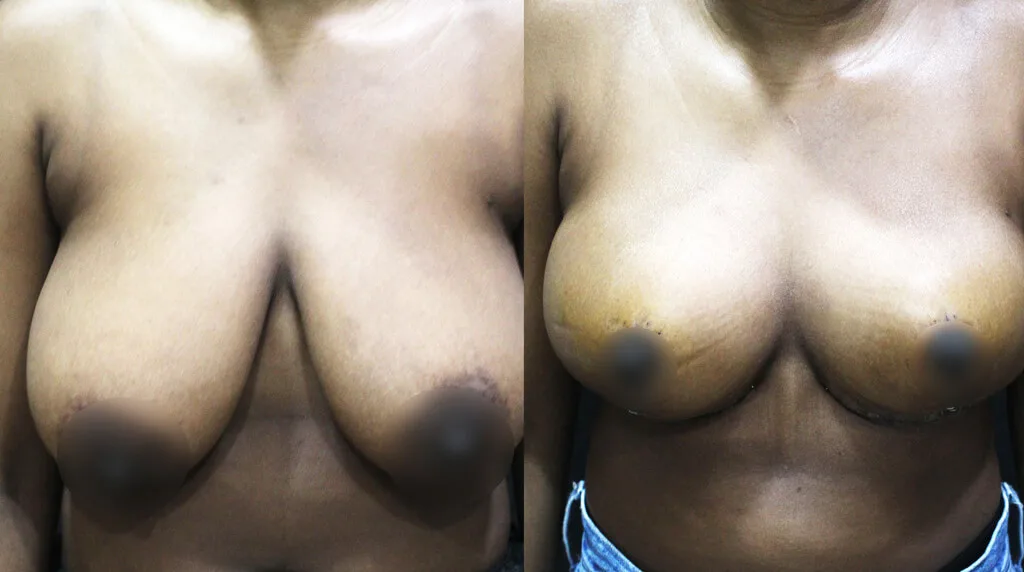
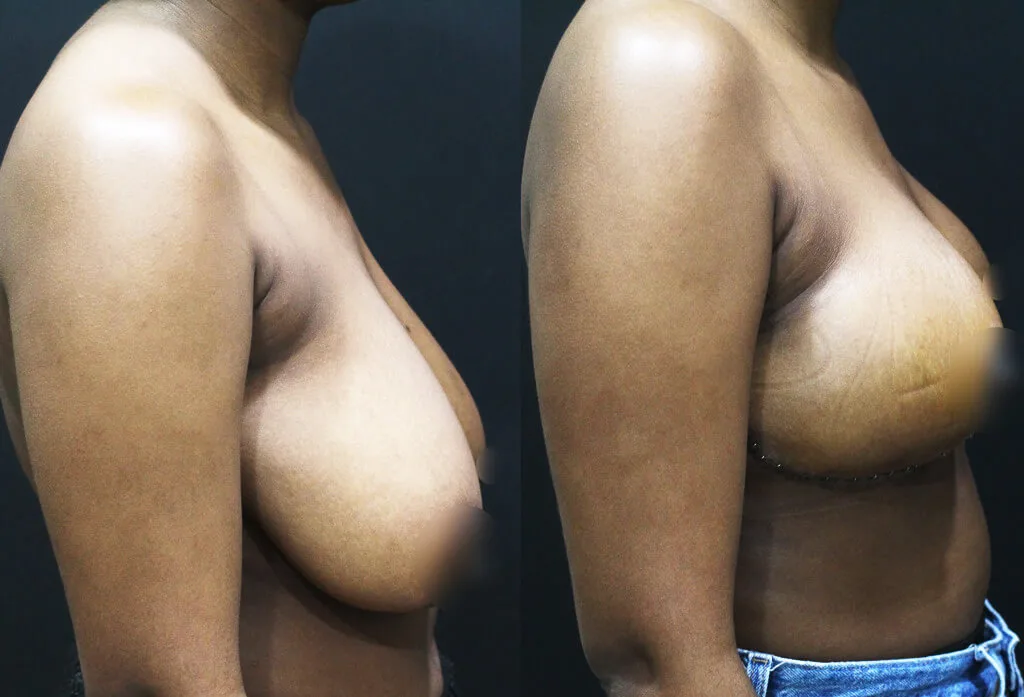
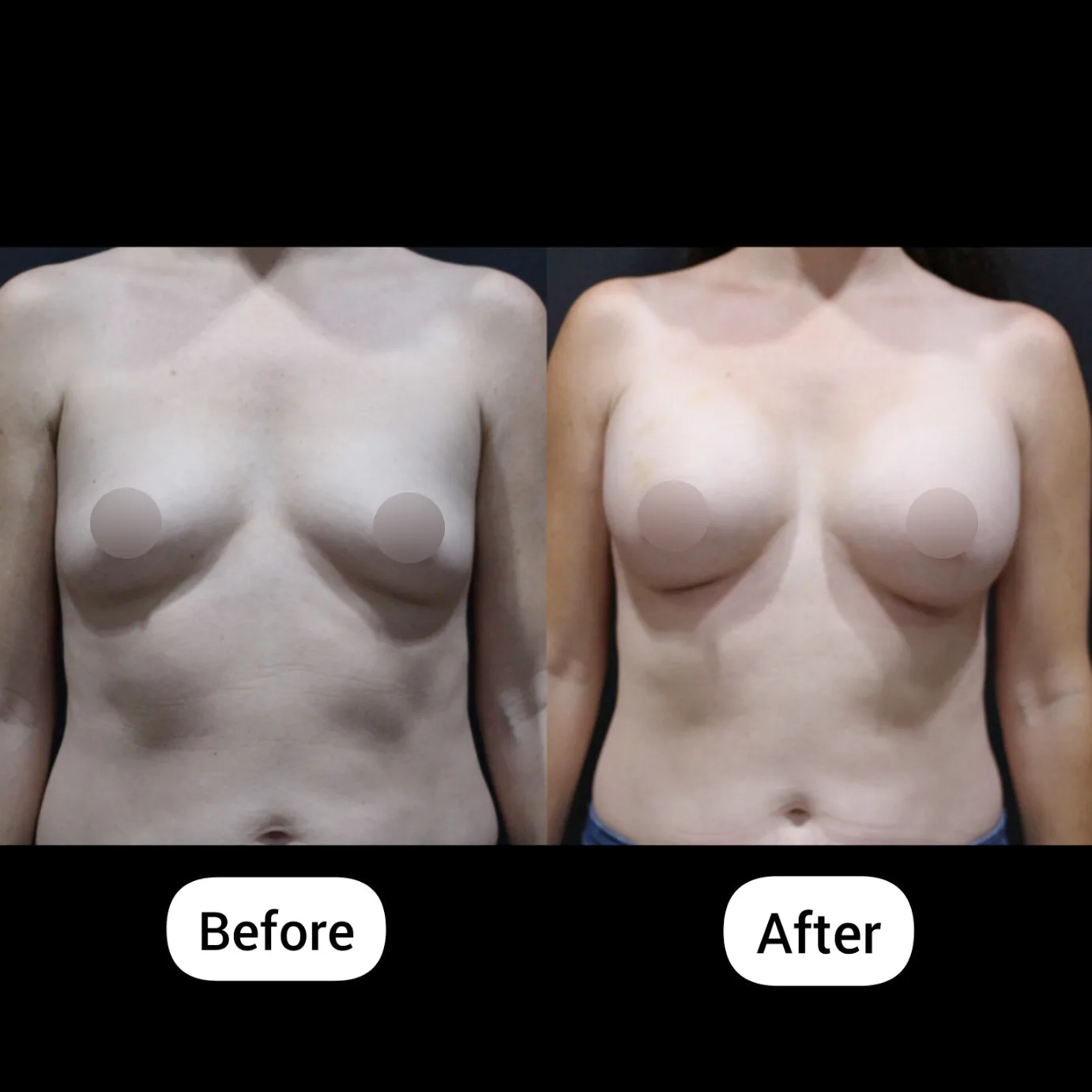
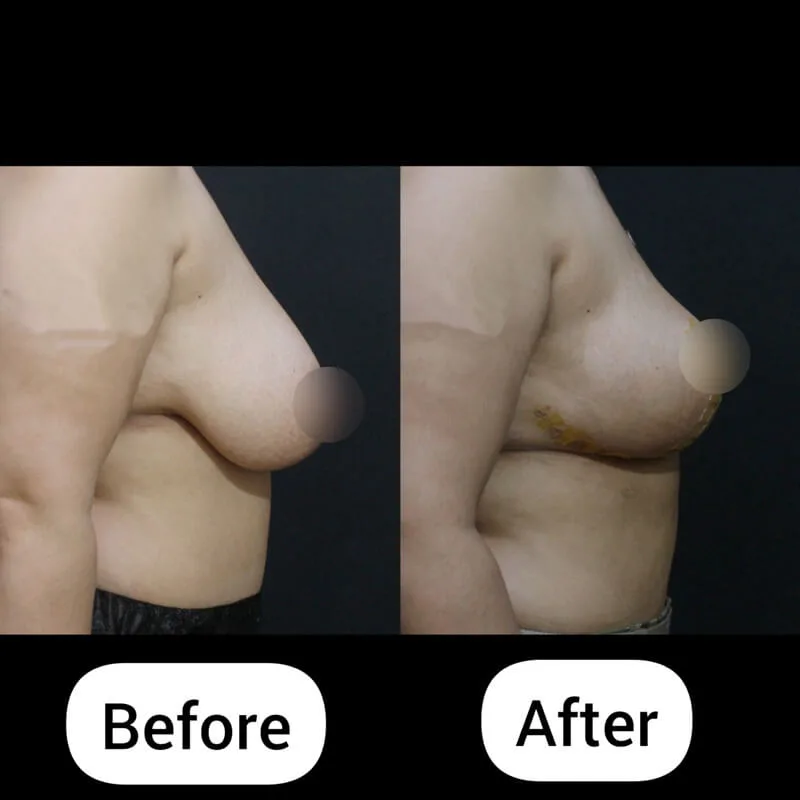
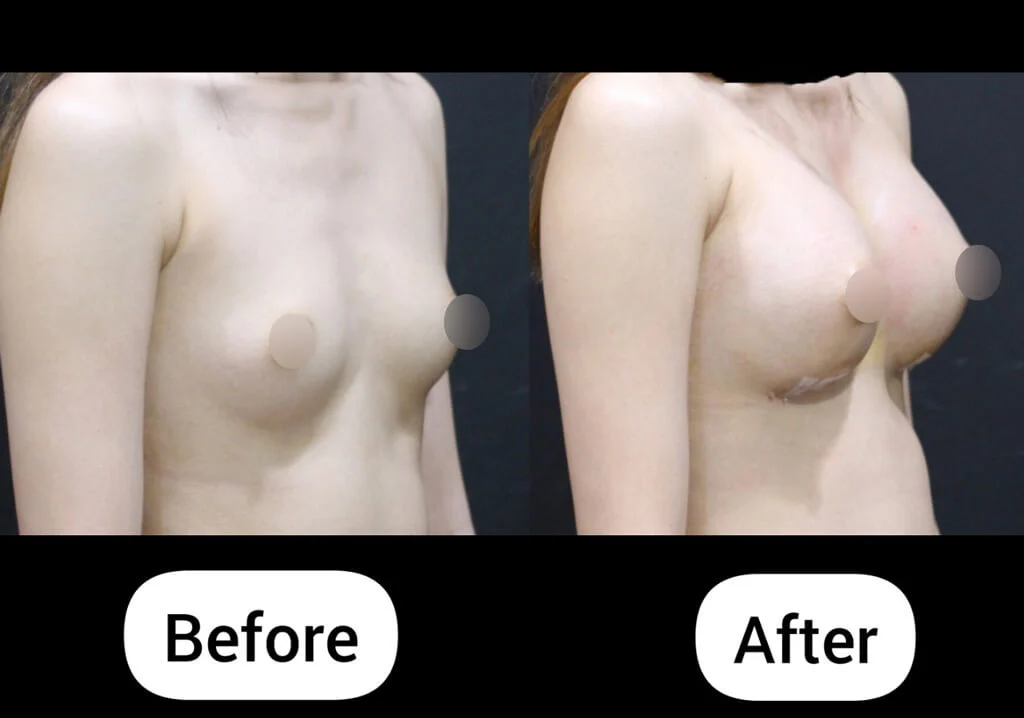
From a Protruding Belly to Visible Definition – 1 Month After Surgery
This patient developed significant abdominal obesity over time due to aging and a sedentary lifestyle, especially long hours of sitting.
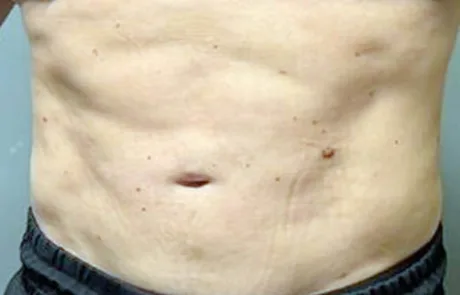
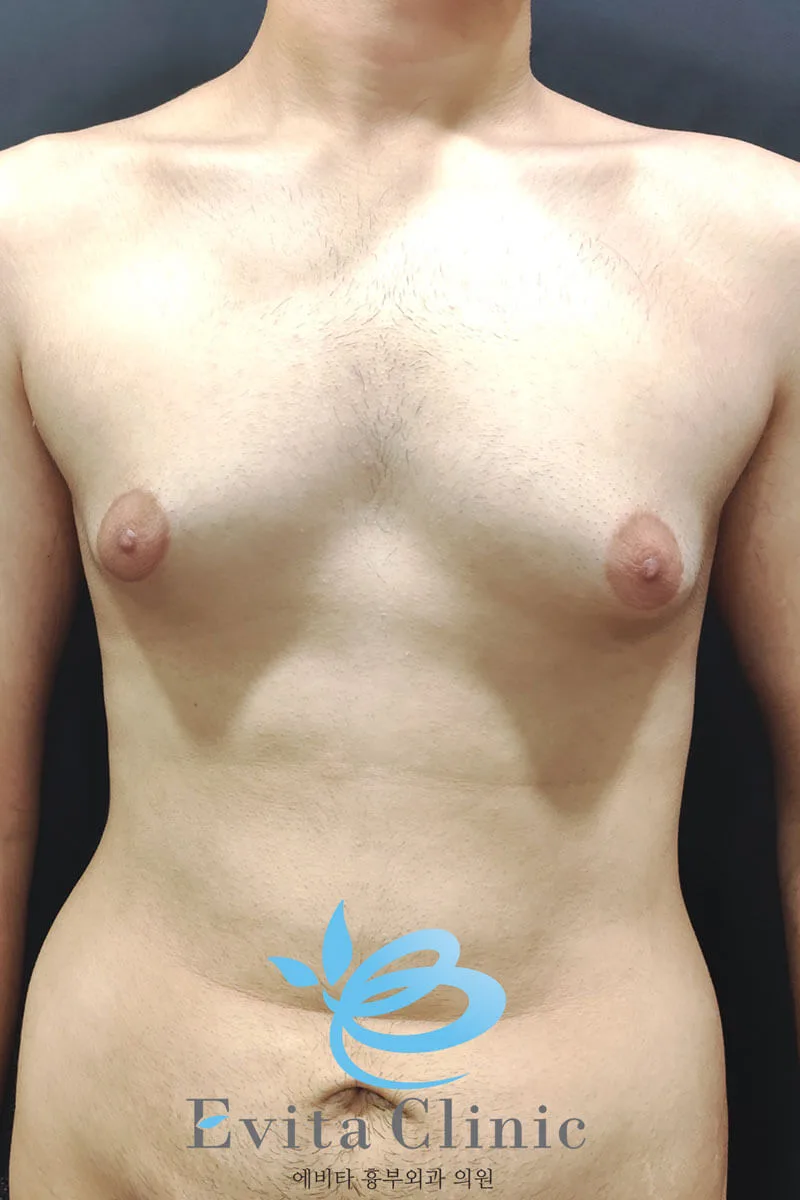
Before surgery, his abdomen showed a typical “protruding belly” shape, mainly caused by visceral fat pushing the abdomen outward.
During consultation, we clearly explained an important medical fact:
Liposuction removes subcutaneous fat (fat under the skin), but it does not directly remove visceral fat (fat inside the abdomen).
Because of this, long-term improvement requires postoperative lifestyle changes and weight control.
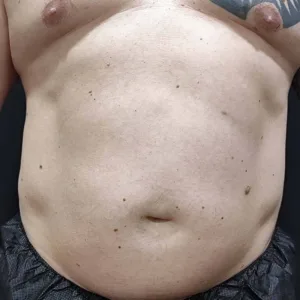
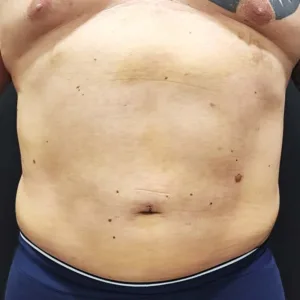
Early Recovery (1 Week After Surgery)
At 1 week post-op, the patient still had noticeable swelling, which is completely normal.
However:
- No significant bruising or bleeding
- Stable recovery condition
- Patient safely returned to his home country
- Sutures were removed locally
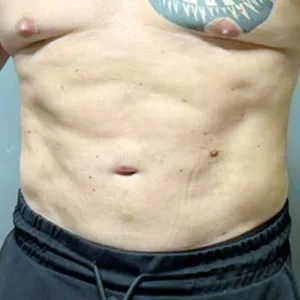
1 Month Result – Noticeable Transformation
One month after surgery, the patient sent us a follow-up photo along with a message of gratitude.
He was very satisfied with the result and even took a mirror selfie in his bathroom to share his progress.
Key improvements include:
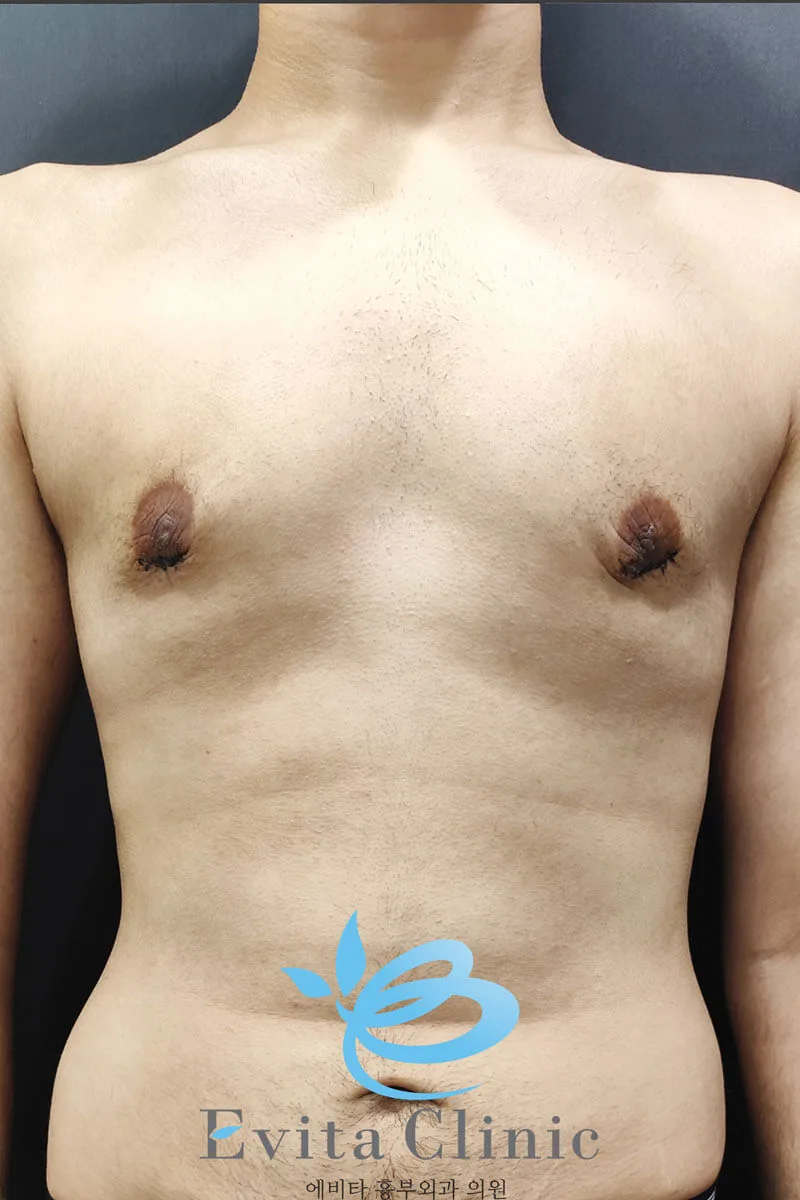
- Significant reduction in abdominal volume
- Emerging six-pack definition
- Improved flank (love handle) contour
- Overall more athletic and structured appearance
This result reflects both:
- Effective removal of subcutaneous fat
- The patient’s continued efforts in body management after surgery
Important Medical Insight
Even though the abdomen is now much flatter, some degree of visceral fat may still remain.
👉 This is why continued diet and exercise are essential to further improve the abdominal contour.
In addition, it is important to note that postoperative irregularities and minor unevenness can continue to improve over time.
The healing and skin retraction process typically progresses over 4 to 6 months, during which the abdominal contour becomes smoother and more refined.
As recovery continues, the overall body shape is expected to become more natural, balanced, and aesthetically defined.
Additional Consideration
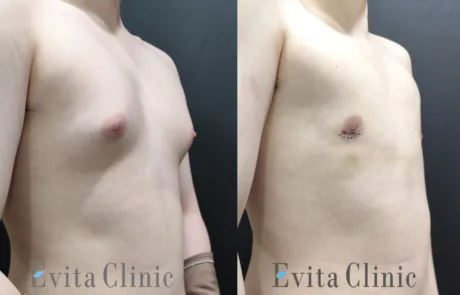
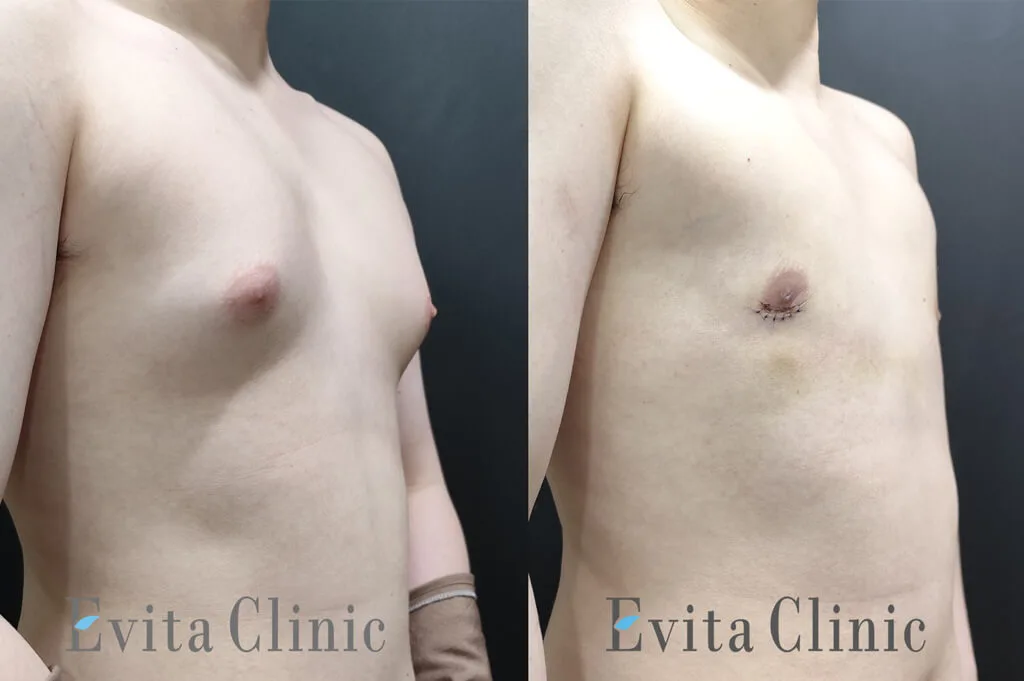
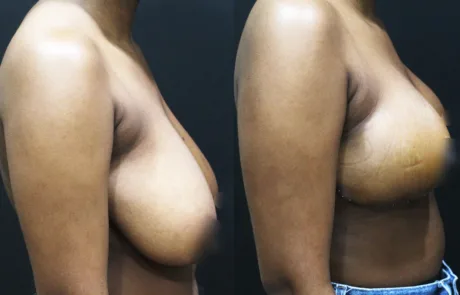
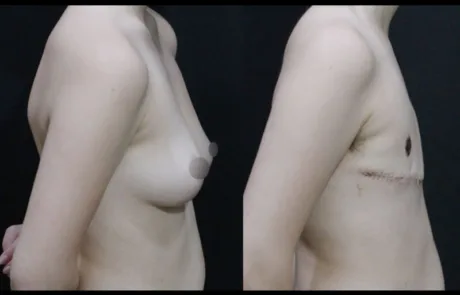
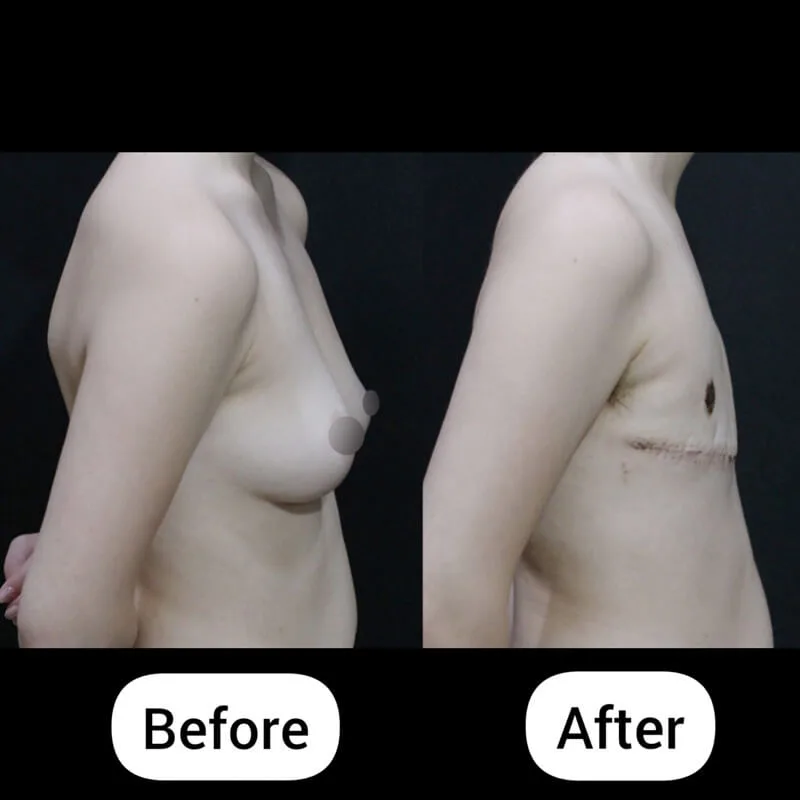
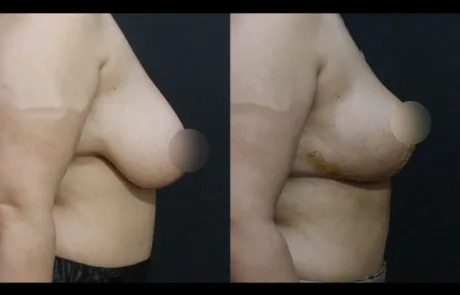
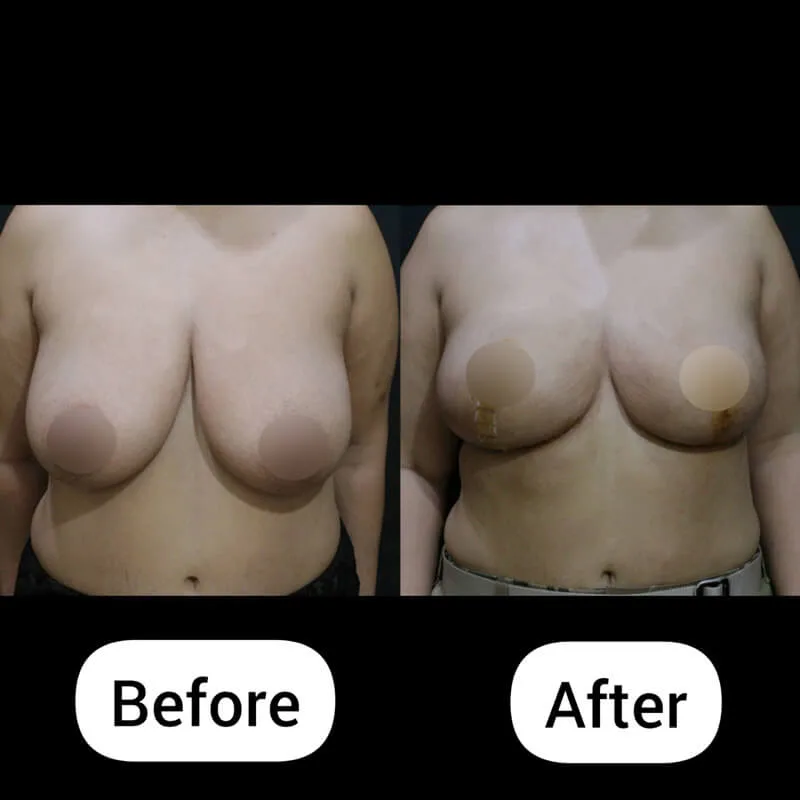
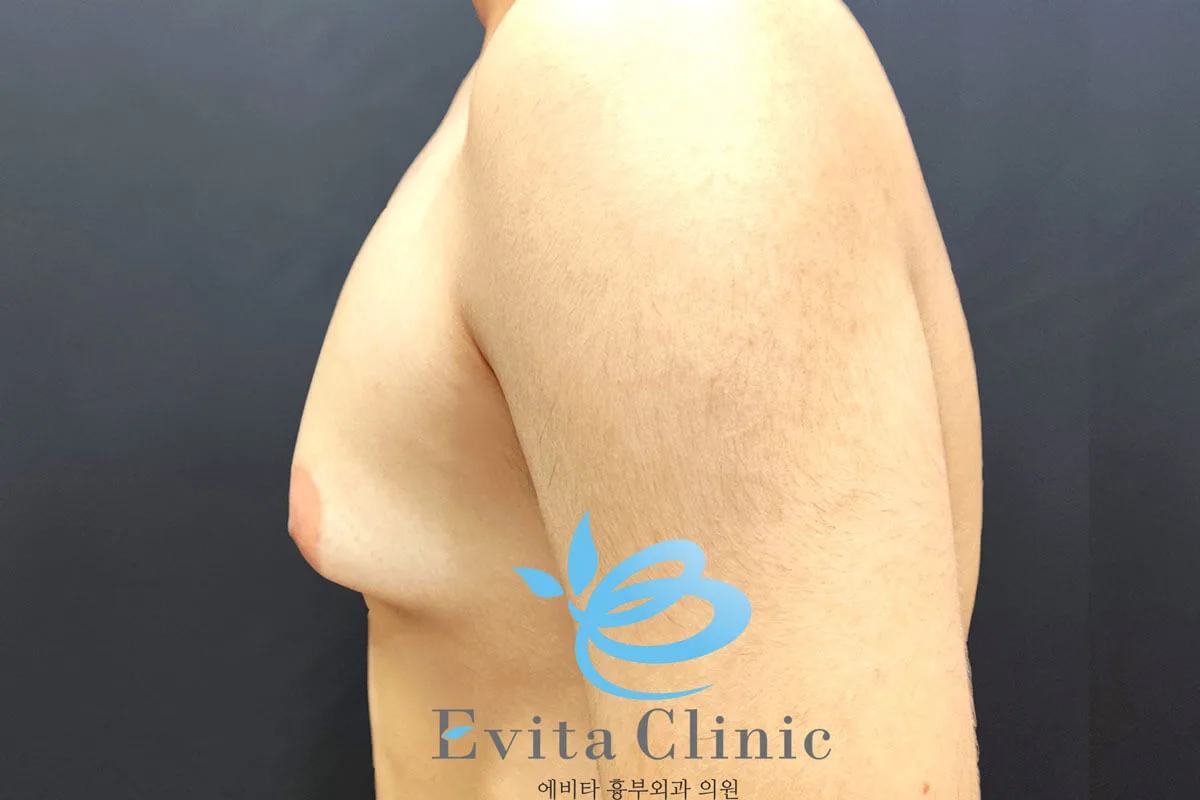
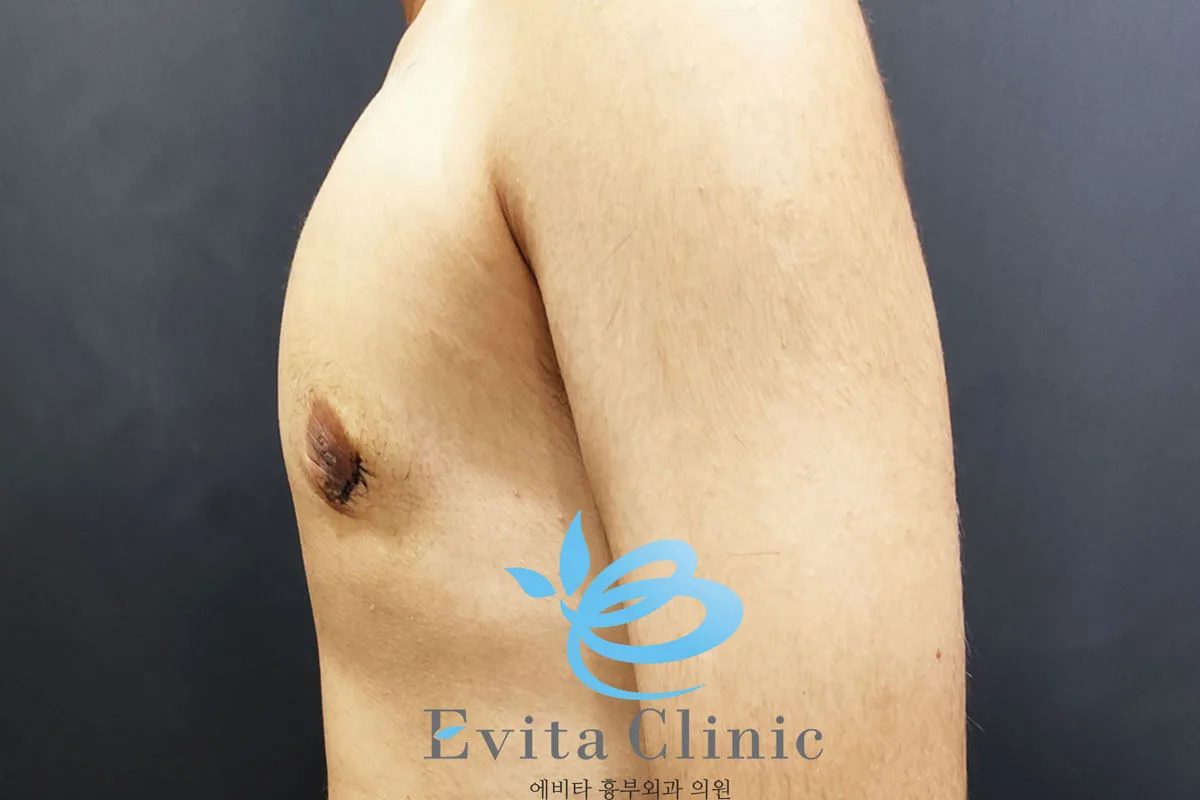
A mild degree of gynecomastia is still visible.
The patient is considering revisiting Korea next year for possible correction.